In recent years, the emergence of drug-resistant bacteria and fungi has become a pressing concern for public health worldwide. These microorganisms, once easily controlled with antibiotics and antifungal agents, have developed resistance mechanisms, rendering these treatments less effective.
This phenomenon, known as antimicrobial resistance (AMR), poses a significant threat to modern medicine. Infections of this type result in increased morbidity, mortality, and healthcare costs.
A Growing Problem:
- According to the World Health Organization (WHO), drug-resistant infections cause an estimated 700,000 deaths each year globally.
- The Centers for Disease Control and Prevention (CDC) reported that more than 2.8 million antibiotic-resistant infections occur in the United States annually, resulting in over 35,000 deaths.
- By 2050, AMR is projected to cause 10 million deaths each year globally, surpassing cancer as the leading cause of death if action is not taken.
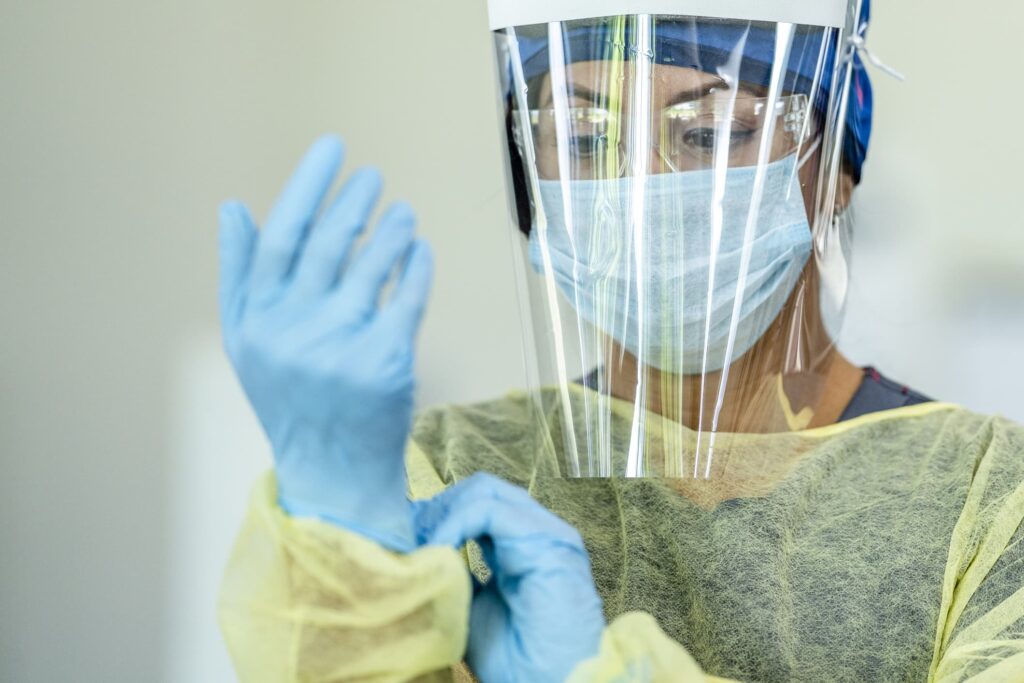
In this article, we’ll touch on the history and challenges of AMR, specific strains of drug-resistant bacteria and fungi, antibiotic stewardship, and personal protective equipment (PPE) specifically designed to prevent the spread of hospital-acquired infections (HAIs) of all kinds.
History and Challenges of Drug-Resistant Strains
The discovery of antibiotics in the early 20th Century revolutionized healthcare by effectively treating bacterial infections. However, the overuse and misuse of antibiotics in both humans and animals have fueled the development of drug-resistant bacterial strains.
The emergence of multidrug-resistant pathogens has further complicated the control of infections in healthcare settings.
Drug-resistant infections can affect anyone, including previously healthy individuals. These infections are particularly concerning for sick patients in hospital settings. Many may have compromised immune systems making them more susceptible to life-threatening infections.
Increasingly, antibiotic-resistant infections are found not only in healthcare facilities but also in community settings. The rise of antibiotic-resistant urinary tract infections, bloodstream infections, surgical site infections, and respiratory infections make it challenging to provide effective treatment.
Fungal infections, such as vaginal yeast infections and invasive Candida auris infections, have also become more difficult to manage due to antifungal resistance.
Importance of Antibiotic Stewardship
Healthcare providers play a critical role in tackling drug resistance by adopting antibiotic stewardship practices. This includes prescribing antibiotics only when necessary, selecting appropriate antibiotics based on the specific pathogen, and ensuring patients complete their full course of treatment.
Diagnostic tests that identify the causative microorganism and its antibiotic susceptibility also help in tailoring targeted treatment, preventing unnecessary or ineffective antibiotic use.
Antibiotic stewardship also means stressing the importance of taking the full amount of properly prescribed medication to completion.
We’ve all heard it before, “I stopped taking my antibiotic or using my antifungal treatment earlier than instructed by my doctor because I felt so much better.”
It’s a tale as old as the medical profession. Unfortunately, this “I don’t want to take something I don’t feel I need anymore” is counterintuitive to full recovery. Patients just sometimes do not understand why the full dose is the full dose. So, even though you say it once, it’s worth repeating — take the full amount prescribed unless otherwise advised by your doctor.
Types of “Superbug” Drug-Resistant Bacteria and Fungi
1. Methicillin-Resistant Staphylococcus aureus (MRSA)
MRSA is a type of bacteria that has developed resistance to methicillin, a commonly used antibiotic to treat Staphylococcus aureus infections. This drug-resistant pathogen can cause a range of infections, from skin and soft tissue infections to severe bloodstream infections. MRSA is often found in healthcare settings, but it is important to note that community-associated MRSA infections have been on the rise.
2. Carbapenem-Resistant Enterobacteriaceae (CRE)
CRE refers to a group of bacteria that have become resistant to carbapenems, which are considered the last resort antibiotics for severe infections. These bacteria primarily cause infections in the urinary tract, bloodstream, and surgical sites. Unfortunately, CRE infections are associated with high mortality rates due to the limited treatment options available as a result of resistance.
3. Candida auris
Candida auris is a type of fungus that has emerged as a significant concern, particularly in healthcare settings. This resilient fungus is often resistant to multiple antifungal treatments, making it difficult to control and treat. Candida auris infections primarily affect individuals with weakened immune systems, causing serious bloodstream and wound infections.
4. Bacteria that produce Extended-Spectrum Beta-Lactamase (ESBL)
ESBL-producing bacteria (such as E. coli) are a group of bacteria that produce enzymes called beta-lactamases. These enzymes render common antibiotics ineffective, leading to treatment challenges. ESBL-producing bacteria commonly cause urinary tract infections, respiratory tract infections, and bloodstream infections. They pose a formidable challenge in healthcare and community settings due to their ability to spread easily from person to person.
5. MultiDrug-Resistant Tuberculosis (MDR-TB)
MDR-TB is a form of tuberculosis that is resistant to two of the most effective first-line antibiotics: isoniazid and rifampicin. Treating MDR-TB requires the use of second-line antibiotics that are less effective and often associated with more side effects. This form of tuberculosis poses a significant threat to public health as it easily transmits and is difficult to control.
Every Effort to Stop HAI Spread of Superbugs Matters
The rise of drug-resistant bacteria and fungi, including superbugs and CREs, poses significant challenges to healthcare facilities and public health. The development and spread of these multidrug-resistant pathogens threaten the effectiveness of antibiotics. The industry should heighten the urgency to implement infection control measures and prioritize proper antibiotic stewardship.
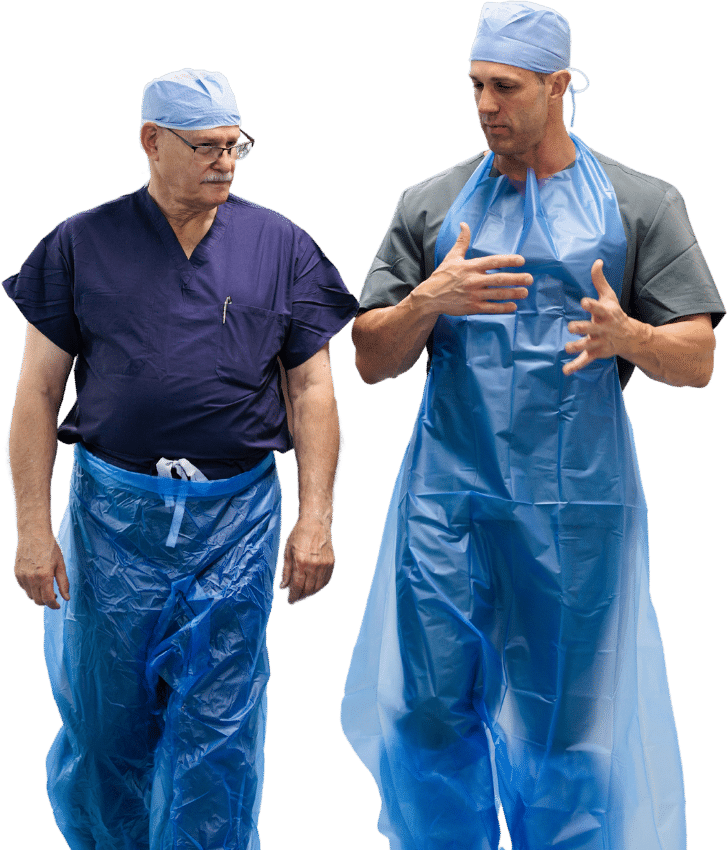
The increased need for personal protective equipment (PPE) to prevent the spread of HAIs means the need for quality materials is higher than ever. Proper donning and doffing are also key in protecting both patients and medical professionals. By utilizing proper hand hygiene, disinfection protocols, and wearing quality PPE, healthcare workers can reduce the risk of transmitting drug-resistant bacteria and fungi within healthcare facilities.
Founder Stewart Sloan designed STA-DRI knowing firsthand how important product quality is when it comes to actually protecting healthcare workers and patients. Specifically designed to prevent the spread of HAIs, including drug-resistant pathogens, we are offering free samples to ensure every surgeon and nurse gets the chance to experience the difference.
By equipping healthcare workers with high-quality PPE and promoting proper infection control practices and antibiotic stewardship, we can safeguard the health of both patients and healthcare providers. Together, we can combat the rise of superbugs and CREs, ensuring a safer and healthier future for all.